Blogs
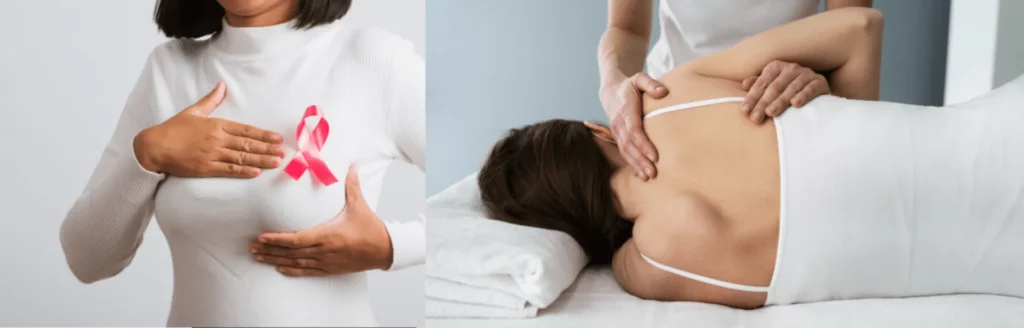
After undergoing a mastectomy, individuals often face a challenging journey of recovery. While surgery is a crucial step in treating breast cancer or reducing the risk of its recurrence, it can also bring about physical and emotional changes. In this post, we’ll explore how post-mastectomy physiotherapy plays a vital role in enhancing recovery beyond surgery. […]
Blogs
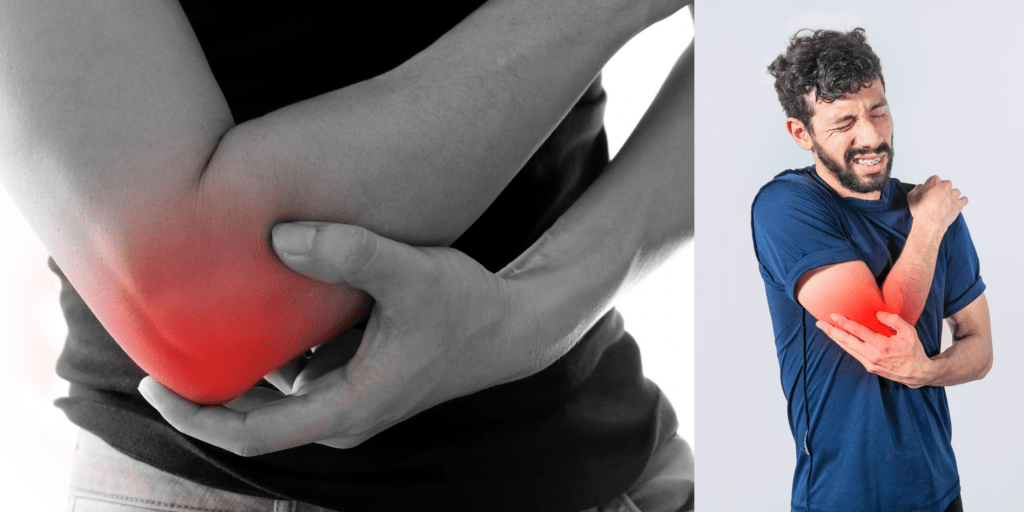
Tennis elbow is a nasty ailment affecting more than just tennis enthusiasts, can be a persistent challenge. At Achieve Health we recognize the impact of this condition on daily life. In this article, we delve deeper into our multifaceted approach, incorporating a range of modalities, including needling, deep soft tissue massage, and detailed exercises, to...

Blogs
When the ankle is twisted or rolled, a common injury that can result is an ankle ligament tear. Numerous ligaments in the ankle help to stabilise and support the joint. Depending on how badly the ligaments have been damaged, ankle ligament tears can range in severity from mild to severe. They have several grades...
Blogs
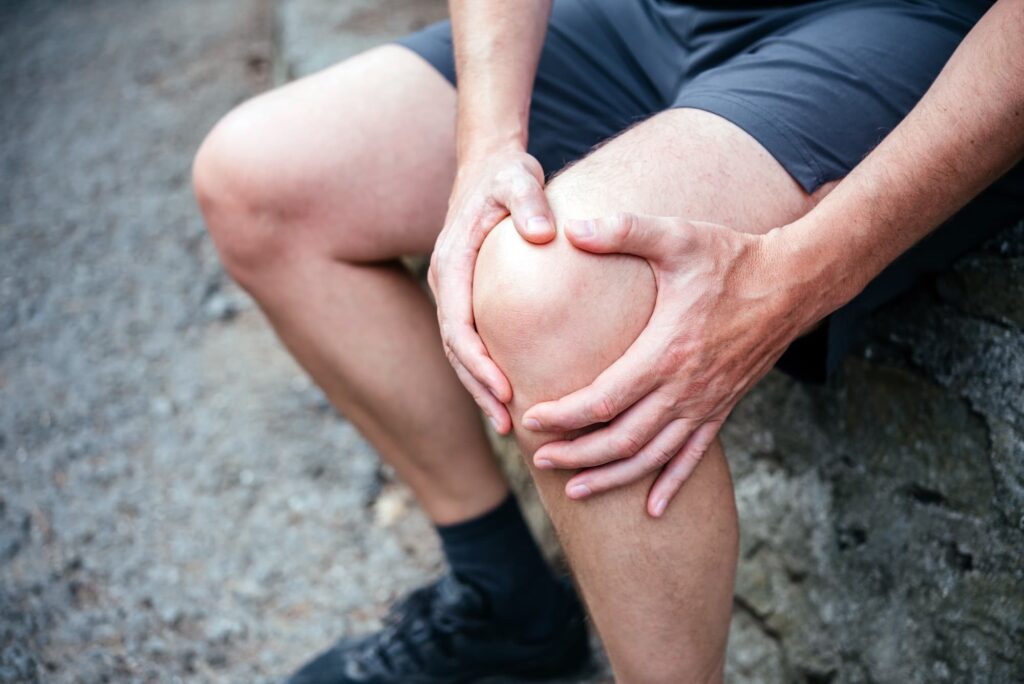
See Case Study below, but first – What is an ACL tear? An anterior cruciate ligament (ACL) tear is a specific kind of knee injury that happens when the ACL is torn. One of the four main ligaments in the knee, the ACL joins the shinbone to the thigh bone (femur and tibia). It aids...
Blogs
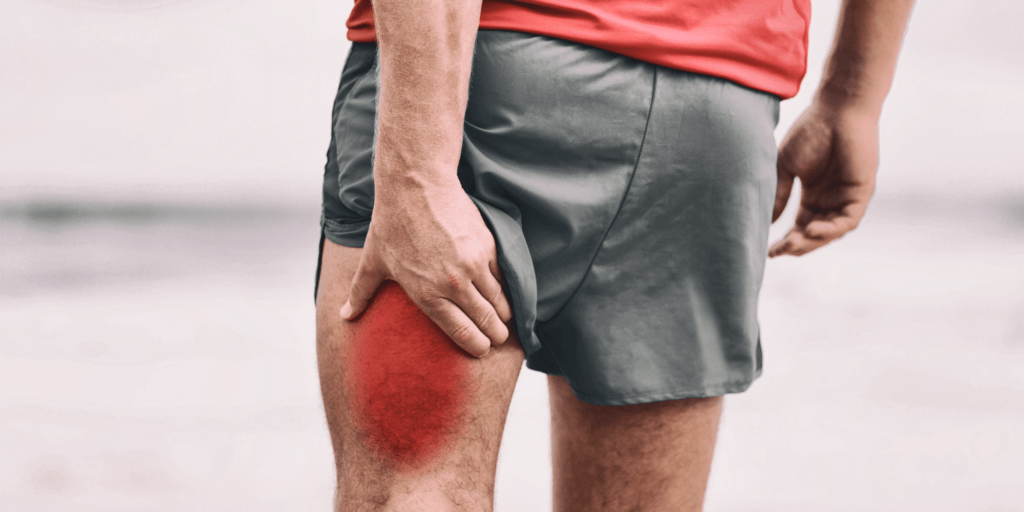
Hamstring Tear When one or more of the muscles at the back of the thigh are stretched above their breaking point, a partial or total tear can ensue. This is known as a hamstring tear. According to the degree of the muscle damage, hamstring tears can range in severity from minor to severe and are...

Blogs
Patellar tendonitis, also known as jumper’s knee, is a common knee condition that affects athletes and individuals involved in activities that require repetitive jumping or knee movements. This condition can be painful and debilitating, but with proper understanding and management, it is possible to recover and return to your regular activities. In this blog,...
Blogs
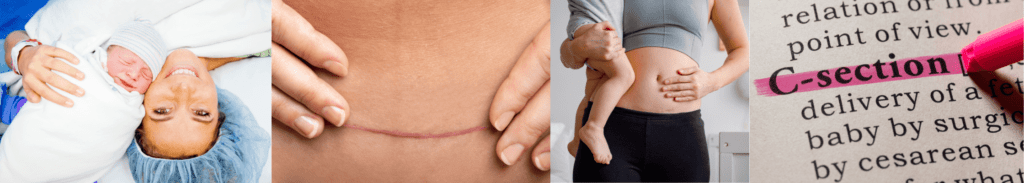
Understanding C-Section Recovery The C-Section Procedure A caesarean section, commonly referred to as a C-section, is a surgical procedure in which a baby is delivered through an incision made in the mother’s abdomen and uterus. While necessary in some cases for the safety of both mother and baby, it involves a longer recovery period compared...

Blogs
Unveiling the Hidden Potential: Exploring the Benefits of Biomechanical Assessment In the realm of health, fitness, and sports performance, the quest for optimization is unending. Imagine having the ability to unlock your body’s hidden potential, enhance your athletic prowess, and prevent injuries before they even occur. This is where the remarkable concept of biomechanical assessment...

Blogs
Achilles tendon issues are common conditions that affects the Achilles tendon, the large band of tissue connecting the calf muscles to the heel bone. It is characterized by pain, stiffness, and swelling in the back of the ankle, often seen in athletes and individuals engaged in repetitive physical activities but it can affect people...

Blogs
The Importance of Injury Prevention Injury prevention is a crucial aspect of maintaining overall well-being, especially for individuals engaged in physical activities or sports. It involves taking proactive measures to minimize the risk of injuries that could hinder daily life, sports performance, or career pursuits. Among the various healthcare professionals who play a significant role...
Blogs
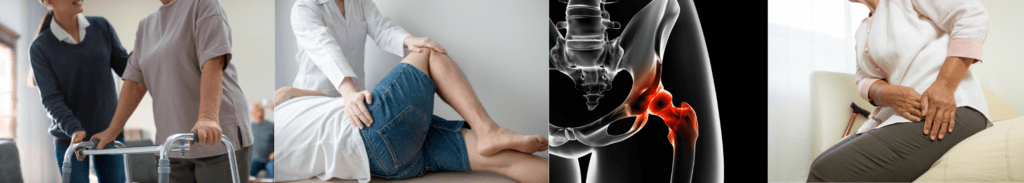
When it comes to total hip replacement surgery, the journey to recovery doesn’t end in the operating room. Physiotherapy plays a crucial role in both the pre-surgical and post-operative phases. In this article, we will explore the benefits of physiotherapy before and after total hip replacement surgery, highlighting its importance in optimizing outcomes and...
Blogs
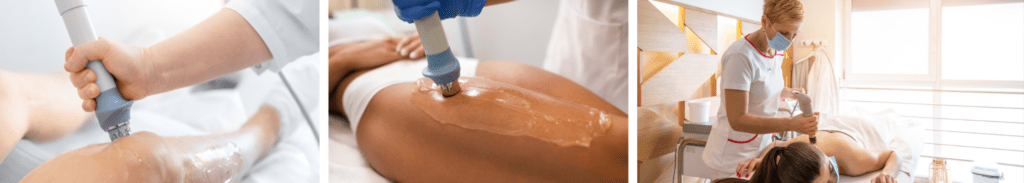
Shockwave therapy is a non-invasive medical treatment that utilizes high-energy sound waves to stimulate healing and provide therapeutic benefits. It has gained significant popularity in recent years due to its effectiveness in treating various musculoskeletal and vascular conditions. This article explores the concept of shockwave therapy, its benefits, applications, effectiveness, safety considerations, and what...
